As temperatures warmed last spring, two expectant women, Katie Plum of Williamsburg and Terrail Williams of Raleigh, North Carolina, gradually prepared for the babies who were supposed to make their grand entrances into the world in several months. Neither knew at the time that their babies would be among the fifteen million worldwide born preterm, and neither could have predicted that the nurses, staff, and other parents at Bon Secours St. Mary’s Hospital Neonatal Intensive Care Unit (NICU) would profoundly impact their emotional and mental well-being during a time of anxiety and uncertainty.

Twelve weeks before her due date, Katie experienced symptoms of early labor and was admitted to a Williamsburg hospital near her home. The staff there quickly transferred her to St. Mary’s so she and her baby could receive the best possible care. As she had hoped, the St. Mary’s NICU staff delayed labor as long as possible to improve the baby’s lung development. On June 1, after about fifteen hours, Audrey entered the world weighing just two pounds and six ounces. Audrey then spent seventy-five days being cared for in the NICU while Katie and her husband, Steve, commuted between Richmond and Williamsburg.
Around the same time, Terrail, who had been pregnant with twins for only twenty-six weeks, traveled from Raleigh to visit her mother in the Richmond area. She went into premature labor and was taken to St. Mary’s. On June 9, she delivered her babies, a son, Sebastian Jamarrcus Hosier, who weighed one pound, fourteen ounces, and a daughter, Trinitee Jewel Hosier, who weighed one pound, ten ounces. Despite the NICU experts’ best efforts, Sebastian passed away shortly after his birth. Trinitee, the tiniest of fighters, stayed in the NICU for 111 days before she was strong enough to go home.
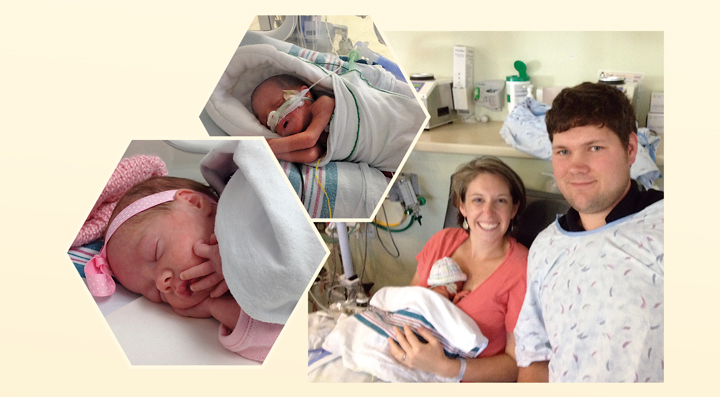
St. Mary’s NICU celebrated its twenty-fifth anniversary on a warm fall day in September, and on that day, it welcomed back many of the parents and babies who have been through its doors since its opening in 1991, like the Williams family and the Plums. According to Denise Smith, NICU nurse manager, Bon Secours first opened the NICU in response to patient need. The staff wanted to keep moms and babies together through labor and delivery in as many cases as possible. Back then, St. Mary’s had only ten beds, and, in some cases, they still had to separate moms and infants, transferring tiny babies to what was then the Medical College of Virginia (now VCU Medical Center).
Over the past twenty-five years, the capacity of St. Mary’s NICU has doubled. It now offers the highest level of care to its patients and is on the receiving end of those transfers from many local hospitals. Smith explains that St. Mary’s rarely transfers babies out to a higher level of care. According to Chief Nurse Executive Nellie League, when they do have to transfer a baby to a VCU or UVA Health System hospital, the babies are transferred back as soon as they are stable enough to stay in St. Mary’s NICU.
As the unit has grown, Smith explains, they have been able to focus on refining what they do, continually working to incorporate evidence-based best practices. Recently, the NICU collaborated with the Children’s Hospital of the King’s Daughters in Norfolk to offer donor breast milk when needed. Other success stories include training parents to perform infant massage, and working to decrease lengths of stay while setting up parents for success at home with their tiny charges. “We constantly ask ourselves,” Smith says, “is there a change we can put in place to make things better for families?”
In response to patient feedback, for instance, the team at St. Mary’s decided in the past five years to keep the unit open all the time instead of restricting visiting hours. “That was a culture change for everyone,” says Smith, “but it is a huge satisfier for families.”
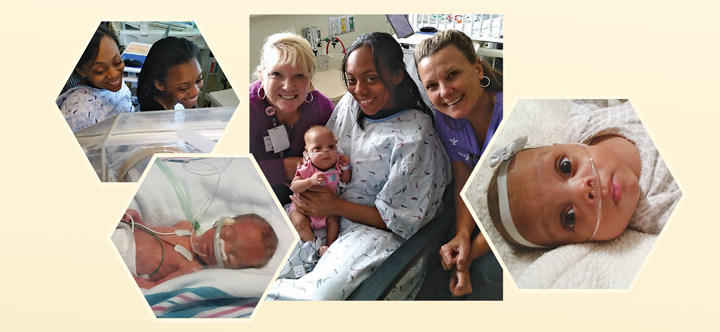
Community partnerships also help to improve parents’ experiences while their babies stay in the NICU. The Ronald McDonald Foundation, for instance, sponsors rooms on-site to enable parents to stay when their babies are critically ill, but the mother has recovered enough to go home. Both Katie and Terrail took advantage of this opportunity and stayed in rooms when their babies were being treated this past summer. Terrail and her husband, Jamaar Hosier, stayed for about a week. As Raleigh residents, the couple was especially pleased with this service. Katie and Steve Plum stayed overnight several times to be closer to baby Audrey. Being able to walk down the hallway to see their babies almost made it feel as if the families were at home, caring for them the way they would have, had the babies been born full-term.
Smith explains, “Life doesn’t stop outside the hospital, so most families have to leave at some point, at least to go home and get a night’s sleep.” To help parents feel connected even when they aren’t there, St. Mary’s developed the bonsecoursnicu.net technology, a camera monitoring system that enables parents to continually and safely monitor their babies on camera. When it was developed several years ago, it was the first program of its kind in Virginia and among the first in the country. The password-protected system also enables long-distance relatives to monitor the progress of the family’s new baby. Recently, Smith communicated extensively with a grandmother who lived halfway across the world to help her bond with her new grandbaby.
Both Smith and League emphasize that being a NICU nurse involves taking care of not just the babies, but the whole family. “We take care of the parents as much as we do the babies,” Smith explains. League also describes the task of guiding families through the range of emotions they feel. “Parents of premature babies,” League says, “grieve the loss of the pregnancy they thought they’d have. We, along with the chaplains and physicians, help them work through those stages of grief.”

Looking back, Terrail and Jamaar spoke about the mixed emotions they experienced during their hundred-plus day stay at St. Mary’s NICU. “The nurses helped me grieve one twin while celebrating the other,” Terrail said. The new mom explained that the team members were always sensitive to her feelings, particularly when other women delivered twins at the unit. “They were always supportive, whether that meant asking questions,
and making sure I was okay, or just letting me be.”
Katie also spoke about the nurses’ awareness of her grief and anxiety during the time her daughter stayed in the NICU. Though she is grateful and fortunate that Audrey survived and is now thriving, the new mom still felt a sense of loss for the pregnancy that didn’t happen as planned, and the nurses were in-tune to that. “They knew they needed to treat not just [baby] Audrey, but the whole family,” she explained. Even the smallest gestures had an impact. For example, Katie spoke about how her daughter’s primary nurse, Sarah, dropped off a box of tissues for her. “As Audrey moved around the NICU, she moved the box or replaced it when needed. Somehow it seemed that all the right people showed up at the right time.”
Both Katie and Terrail mentioned how the staff’s calmness helped them feel at ease. “Families would walk in, balancing life and death,” Katie explained. “The team worked professionally together, problem-solving any challenge, calmly and quietly, even during emergencies.”

The NICU camera and the staff’s calmness and competence enable parents to walk away, trusting that the nurses know what they’re doing. “The hardest day is when the mom has to leave,” League says. “We don’t take lightly that they trust us.” Jamaar Hosier and Steve Plum, for example, had to leave the NICU to return to work, and Katie commuted to the hospital every day from her home in Williamsburg after she was released. Jamaar talked about how staff helped him return to normal life while his daughter still fought for her life. “The nurses left notes each day, and updates about how the baby was doing,” the new father said. “That made me feel okay that I couldn’t be there with her every day.”
At St. Mary’s Hospital, the Evelyn D. Reinhart Guest House also provides respite for the parents of NICU families. Here, once a month, teenage volunteers make dinners for NICU families. Having the chance to get away from the hospital, talk together, and cry together alleviates some of the parents’ stress. “The camaraderie among NICU families is very tight. Moms look out for each other,” Katie said. She described the times she spent with other parents, like Terrail and Jamaar, as an escape from the anxieties she felt about her daughter’s well-being.
For Terrail, that camaraderie with the other parents and nurses has been a life-changing experience. The bonds she developed enabled her to experience social interaction during those difficult months when she was hours from her Raleigh home. “Every time I got there,” Jamaar said, “all the nurses knew her. She was one of them, and she was able to have a relationship with them.” Terrail talked to the nurses about everything, even career choices, and, because she was there for more than a hundred days, she became a resource for new parents coming in.

While the challenges of giving birth prematurely, losing a baby, and watching a baby struggle for life are innumerable, the parents there, particularly Katie and Terrail, focused on all they have gained from their experience with St. Mary’s NICU. Katie highlighted specifically the opportunities they had to connect with numerous specialists and experts. “It was like a crash course in parenting,” she said, with access to different professionals who teach everything from how to give warm swaddle baths and infant massage to setting up sleep and feeding schedules. “By the time I left, I felt so confident to bring this child home,” said Katie.
Terrail and Jamaar also expressed the confidence they felt leaving the hospital. “We participated in every aspect of her care,” Terrail explained. “She went home on oxygen, but we got extensive training to help her.”
As League explains, during those first weeks and months of watching their children hold on to life so tenuously, the staff and parents form bonds that forever change them. If Terrail and Katie are like the many other parents whose babies have spent time at St. Mary’s NICU, years from now, they will attend reunions with their children, like the one in September, showing them where they got their start in life and connecting them with the staff members who helped them transition from life inside the womb to the outside world. Like many other alumni families, they will send Christmas cards or return to the unit to visit with nurses on birthdays. They may even invite their nurses to special events, like graduations and weddings.
Listening to League reflect on her time helping families as a nurse in the St. Mary’s NICU, she sums up why this facility is so much more than a medical facility where babies are born too soon. “They come to us at the most vulnerable point in life. We have an opportunity to impact them for a lifetime.”





